#IWD2024 | Breaking world records and gender barriers
Ultra-high field MRI is unveiling a picture of endurance, and helping to uncover the physical, social and emotional effects of Associate Professor Donna Urquhart’s incredible Antarctic ultramarathon to empower women and girls.
Harnessing physical and mental resilience to finish an Antarctic ultramarathon
Monash University pain and musculoskeletal researcher, A/Prof Donna Urquhart is pushing past physical limitations, unveiling the intricate connection between mind and body, with a crucial mission to empower girls and women in sports.
Donna made international headlines in January, after crossing the finish line of the longest ultramarathon in a polar region in history.
As the first woman to conquer this challenge, she ran 1,402km over the space of 28 days at the Union Glacier Camp in Antarctica – the coldest, windiest and driest desert on earth.

Donna said she wanted her run to be more than a record, using the attempt to launch a mission to empower young girls and women to love and discover what’s possible for them in sport, and break down the barriers to participation.
“The alarming statistics show that girls can find sport stressful, and by the age of 15 only 32% are still playing, leaving so few to benefit from the enormous physical, social and emotional aspects of sport,” Donna said.
It took a team of volunteers and two years of training, but Donna said pushing her physical limitations was only half of the battle, emphasising the crucial role of psychological strength in overcoming challenges – with the start of her run posing the most significant hurdle.
“When I first arrived in Antarctica, it was overwhelming. I didn’t know if I could live in a polar region and ultimately run 1,300km,” Donna said.
She had set a goal to run 50km per day, but by the third day in, the enormity of this challenge hit hard and suddenly, with Donna forging through minus 20-degree 80km per hour winds and limited visibility.
Donna said the physical risks presented by these conditions such as stumbling and falling, hypothermia, polar thigh, frost bite and knee and foot pain, significantly impacted her confidence at the start of the ultramarathon.
“That first week was so intense – it was a steep learning curve, and I had the realisation that my own initial lack of confidence mirrored the uphill battle women and girls face in sports,” Donna said.
“By pushing my own physical boundaries in this world-record attempt I want to show young girls and women what’s possible when you harness the power of the body and mind.”
“Confidence and self-belief were two emotions that I struggled with early, but this world record run taught me strategies that helped me push on, and I can’t wait to pass this knowledge onto other young women,” Donna said.
Ultra-high field functional imaging is charting new territories in extreme endurance and physical exercise
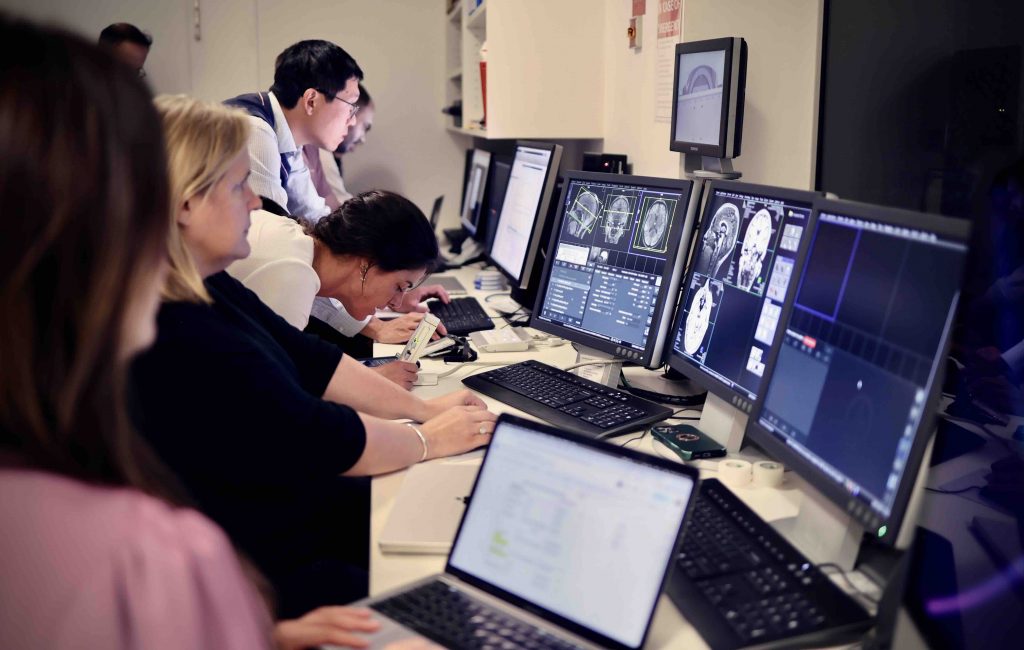
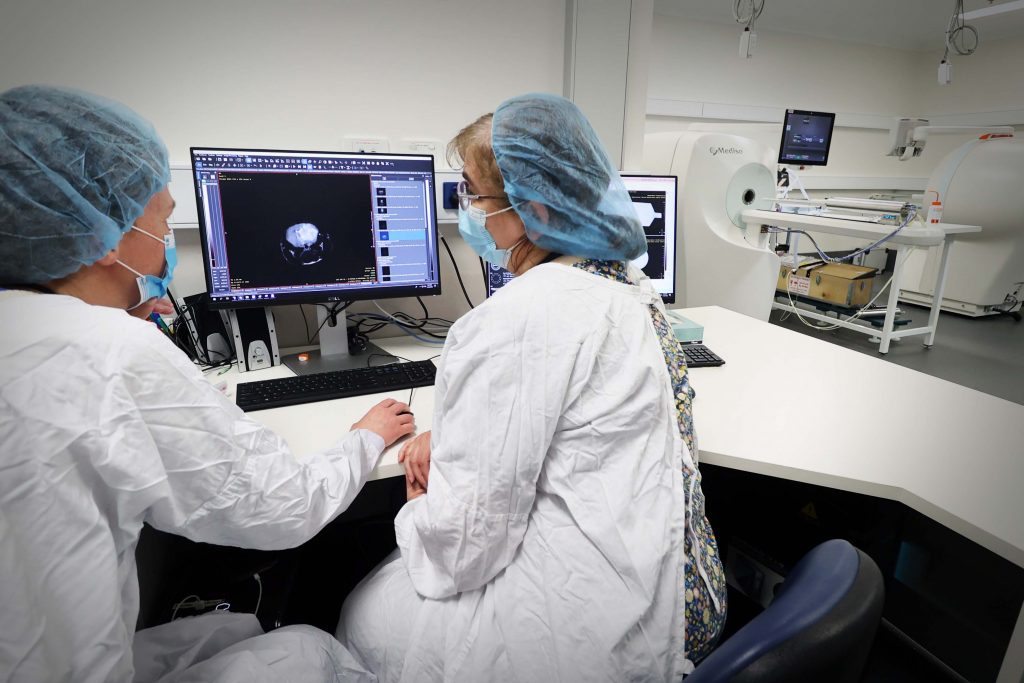
[Pictured: The multi-disciplinary imaging research team, including A/Prof Valentina Lorenzetti, Dr Chao Suo, Dr Hannah Thomson, Ethan Murphy, Anastasia Paloubis, and Arush Arun, with the assistance of University of Melbourne Lead MRI Radiographer Rebecca Glarin, are using imaging to examine the neurological and psychological effects on Donna during this exceptional feat.]
A multi-disciplinary research team is using imaging to examine the neurological and psychological effects on Donna as a result of this exceptional feat, led in collaboration between Donna and A/Prof Valentina Lorenzetti, Lead of the Neuroscience of Addiction and Mental Health Program and Deputy Director of Australian Catholic University’s Healthy Brain and Mind Research Centre, and Dr Karyn Richardson, Wilson Foundation-Brain Park Research Fellow from Monash University.
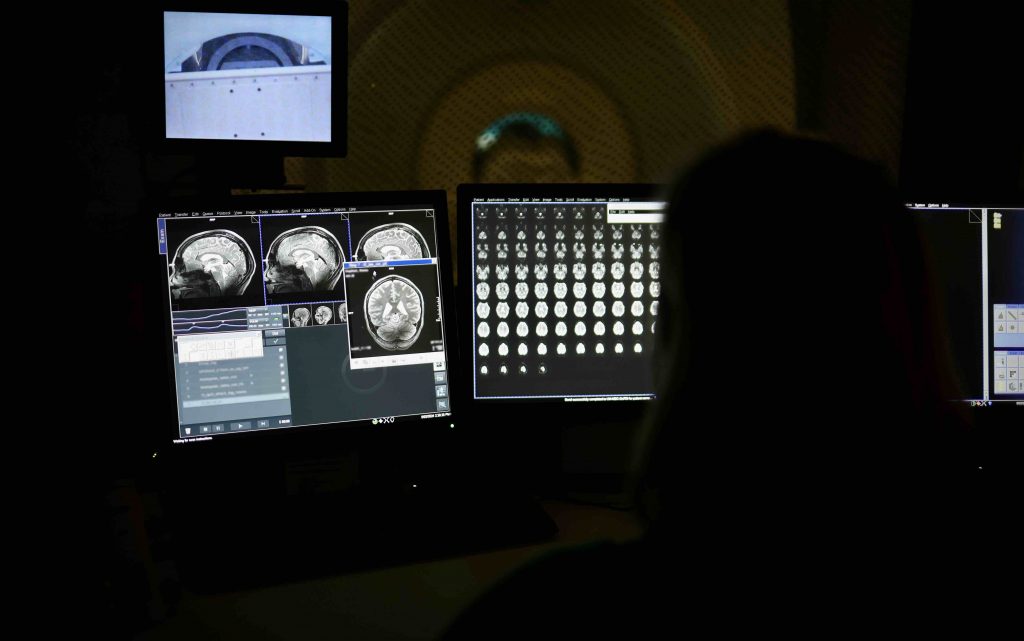
Valentina leads the research team scanning Donna in collaboration with the University of Melbourne Brain Centre Imaging Unit (MBCIU) on NIF’s ultra-high field Siemens Magnetom 7T MRI.
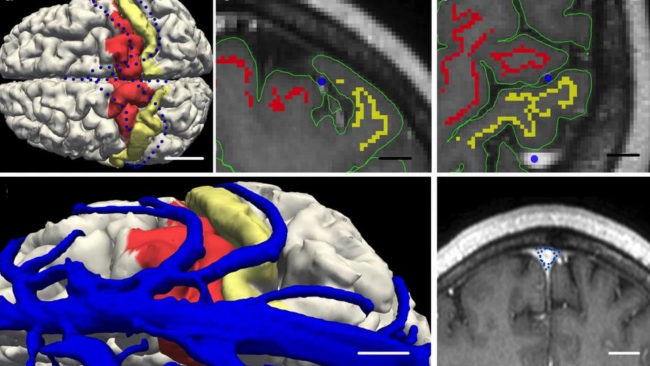
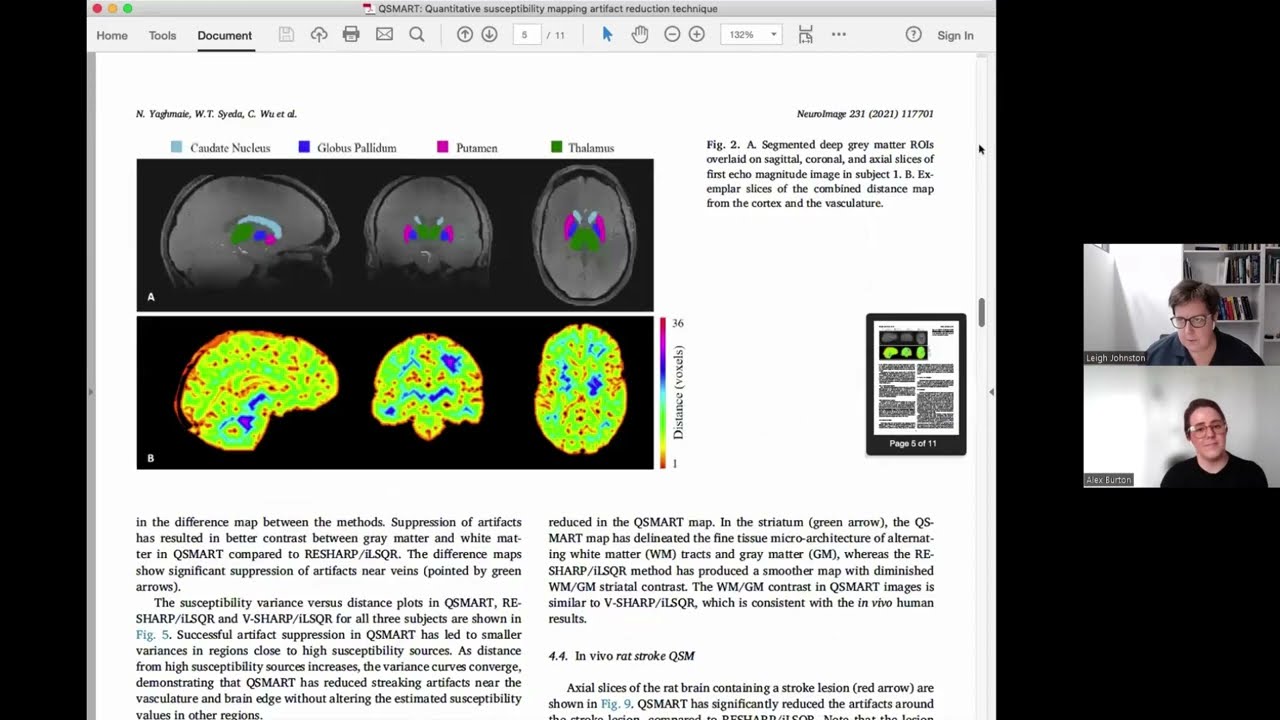
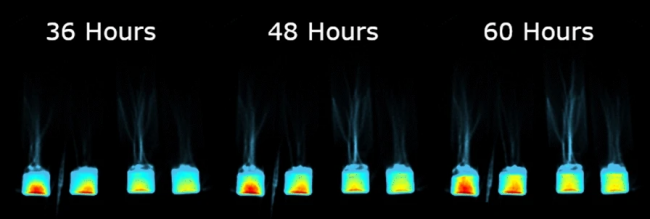
Donna’s exceptional achievement provides an exclusive opportunity for researchers to examine how her brain has changed pre-to-post polar ultramarathon; the 7T MRI can image brain function at a higher resolution than what could be captured on a traditional MRI scan.
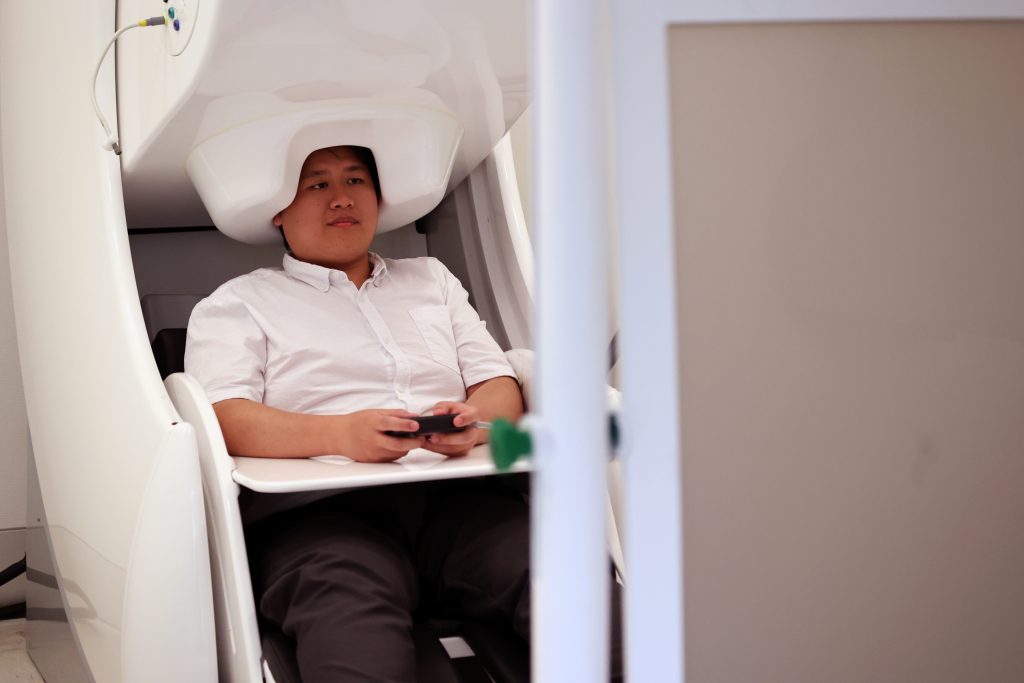
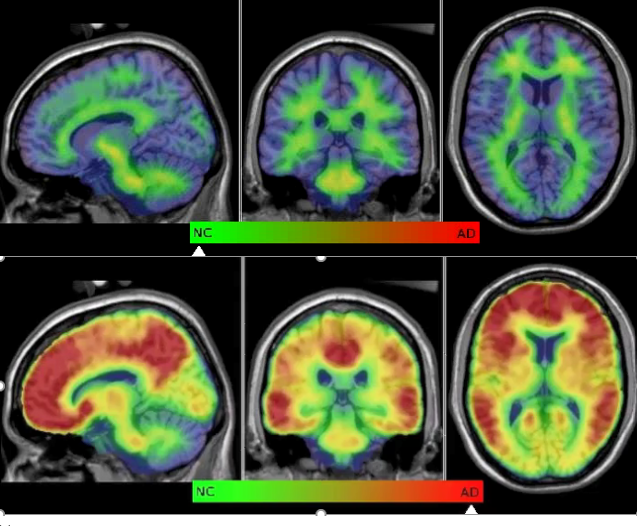
[Pictured: Donna’s brain was scanned with the highest resolution anatomical sequences.]
Donna was scanned twice before the ultramarathon to account for measurement errors, and twice after the ultramarathon (about 2 weeks and 4 weeks), with the highest resolution anatomical sequences, combined with a state-of-the-art functional MRI scan to map the brain networks during rest.

[Pictured: Research imaging team lead A/Prof Valentina Lorenzetti and NIF University of Melbourne Lead MRI Radiographer, Rebecca Glarin]
Valentina said this series of scans can help to provide preliminary evidence on the brain changes that accompany extreme efforts when pushing the body and mind during an ultramarathon in an extreme climate.
“What Donna has done is amazing, and we need examples like this. Everyone knows that exercise is good for you – and now we have the opportunity to showcase the MRI brain images to help convey the message effectively,” Valentina said.
Bridging the mind-body gap: Understanding neurological and psychological insights
Complementary to the imaging study, researcher Dr Karyn Richardson led a mental health and wellbeing assessment to explore how Donna’s mental state changed before and after the event, and how these factors impacted her performance.
Karyn said mental state plays a powerful role in sport, exercise, and endurance and this was a wonderful opportunity to explore these relationships.
Donna completed a variety of questionnaires before and after the ultramarathon to document her general wellbeing, stress and anxiety, coping and confidence.
She also rated a number of factors including pain, confidence, wellbeing, resilience and perceived stress daily in Antarctica, which helped her team to provide additional support during the challenge.

“The data mirrors Donna’s recount of the experience, with a significant period of adjustment over the first week of the run before she acclimatised to the environment and her body adjusted to the daily challenges,” Karyn said.
Karyn said the more confident Donna felt before her run, the quicker she completed the 50km for the day.
“Research has shown that resilience, belief in yourself, and the ability to push through physical challenges are incredibly important for these types of activities, and this is precisely what Donna has done.”
“Donna’s achievement is truly remarkable and her passion to use her experience to inspire young women in sport has blown me away – she is an incredible role model in- and outside of sport,” Karyn said.
Redefining sport for women and girls: Embracing a holistic narrative beyond physicality
The Run Antartica initiative is creating social impact by raising awareness about females’ experience of sport, providing education on a holistic approach to sport, and raising funds for their charity partners, including in disadvantaged communities. Research shows that girls can find sport ‘stressful’ and that 50% stop participating during adolescence (aged 15-19 years). The reasons teenage girls withdraw from sport are multifactorial, however, one of the major contributors is having a lack of confidence.
“This research adds another layer to highlight that sport is about your body, but also about how you train your mind to address the cognitive and emotional components of sport and activity,” Donna said.
“We really see this as a pivotal time in history to evaluate the model we use to look at sport, and change the conversation from focusing on physicality to encompassing a holistic view.”
“We require a comprehensive framework, with a focus on educating young females in the development of cognitive, emotional and social skills in a sporting environment. Our professional athletes are provided with this approach – why aren’t our young people?” she said.
Donna’s mission to empower women and girls in sports aims to disrupt these historical trends which have contributed to dropout rates. In navigating this extraordinary feat, Donna is reshaping the narrative by which we view community-based sport in Australia, empowering the next generation of female athletes to develop a love of sport, and experience the important health and education benefits.
For more information about Donna’s mission or to donate, visit https://www.runantarctica.com/
This research was conducted using NIF expertise and 7T MRI facilities at the Melbourne Brain Centre Imaging Unit at the University of Melbourne.